Gum disease explained
 We outline everything you need to know about gum disease in order for you to recognise symptoms quickly and prevent any associated health issues escalating out of control.
We outline everything you need to know about gum disease in order for you to recognise symptoms quickly and prevent any associated health issues escalating out of control.
What is gum disease?
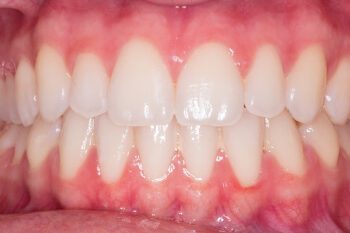
Gum disease is the reversible inflammation of the gum around the teeth, which is caused by dental plaque bacteria. In health, the gums are firmly attached to the teeth and bone underneath, and often appear pale pink and stippled. If you have gum disease the gums appear red, swollen, angry and inflamed. They may bleed when brushing and can be tender or itchy to touch.
For most people, early gum disease (also known as gingivitis) causes no pain, and you may not even know you have it. If left it can progress deeper to more severe forms of gum disease (periodontitis – where the supporting bone and gum fibres become severely damaged), which ultimately leads to tooth loss.
What causes gum disease?
Gum disease is caused by plaque which is the sticky film of food debris and bacteria that accumulates between or around the teeth, especially collecting in hard-to-reach places. The bacteria naturally produce toxins (poisons) and other substances leading to gum infection and inflammation. If this plaque is not removed daily, it will harden to form calculus (or tartar). Calculus can simply be thought of as mineralised plaque, and as it is rough and adherent it will attract more plaque leading to a “vicious cycle of disease”.
Who is affected by gum disease?
We know that more than 90% of the population at some stage will suffer from gingivitis, and more than 50% of the population will have periodontitis in their lifetime at any one time so, it is incredibly common!
Certain patient groups are at higher risk of suffering from gum disease:
- Smokers. Smoking is the biggest cause of gum disease. It cleverly masks the early warning signs of gingivitis as nicotine stops bleeding.
- Diabetics (especially if their diet is poorly controlled)
- Pregnant women or patients on certain birth control pills tablets (relates to hormones modifying the gums).
- People taking certain medications. Certain doctor prescribed drugs can cause gum overgrowth and negatively impact gum health, such as anti-epilepsy medicines (like Phenytoin), Cyclosporin and Calcium channel blockers (like Amlodipine, or Nifedipine).
Even though we have said it is incredibly common, it is rarely managed early. It is a silent condition that has little impact on day-to-day life, and often with little to no pain), much like diabetes or high blood pressure. Therefore, it is important to watch out for some early warning signs.
Early signs of gum disease
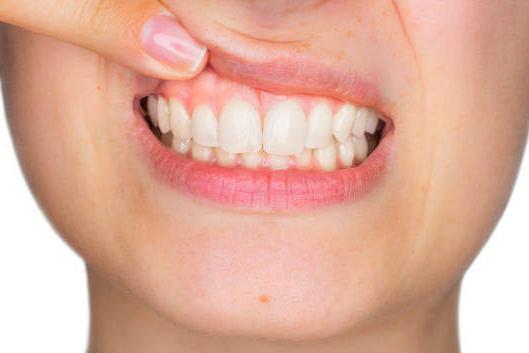
If detected early, gum disease can be reversed. When you see your dentist, be sure to mention any of the following signs to them:
- The gums appear red or even deep purple around the gum margin,
- The gums appear swollen and puffy, angry, and inflamed.
- The gums bleed when brushing or spitting out (pink blood in the sink after spitting out).
- The gums are tender (or itchy) to the touch.
Remember though, the gums can have no obvious symptoms at all so regular dental assessment to diagnose is essential.
Signs of advanced gum disease:
- Gum recession – teeth that look longer as gums have receded due to lost attachment (“long in the tooth”).
- Gum pocketing – gums have detached or pulled away from the tooth creating a gum pocket.
- Drifting or mobile teeth, or changes in the way your teeth bite together – can indicate loss of support for your teeth from the gums.
- Pus from gums.
- Bad breath or a bad taste in your mouth.
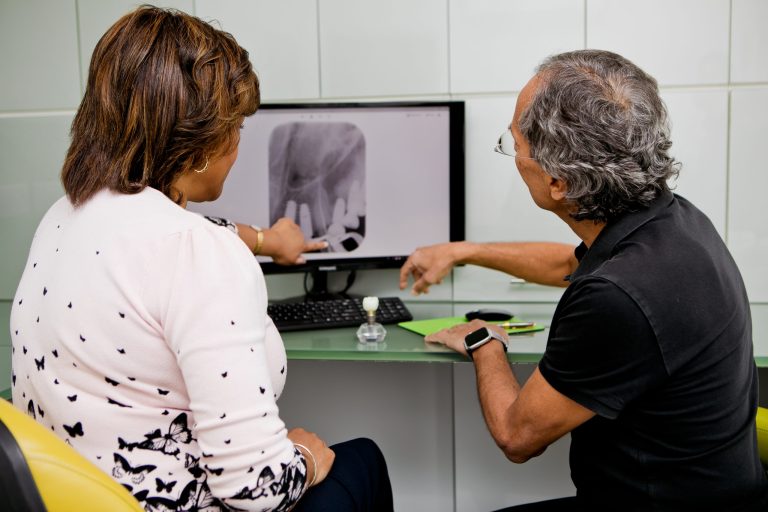
How does the dentist check for gum disease?
Your dentist or hygienist will assess your gums by using a gum probe to see how well your gums are attached to your teeth. They will also look for calculus (or tartar) deposits on your teeth, staining and roughness of teeth, and fillings (particularly around and under the gum line).
The dentist will normally record a severity scores for each areas of your mouth (usually by splitting the mouth into six regions – known as sextants), with each scored from 0 to 4 (0 representing health at one end and 4 representing advanced disease at the other end of the spectrum). This scoring is known as a BPE (Basic Periodontal Examination) and scores of 3 or below can normally be manged by the hygienist or dentist, whereas scores of 4 (advanced disease) may need further expert care by specialist referral.
How long does it take to treat gum disease and how is it treated?
Gingivitis can completely disappear within a week of instituting an excellent twice daily oral hygiene regime. This should include twice daily general toothbrushing (ideally electric but can be manual brushing) and using interdental aids (like floss, interdental brushes) along with specific brushes and techniques that you will learn from your periodontist (gum expert or specialist), hygienist or regular dentist.
If you already have plaque and calculus build-up it is likely that you will need a dental professional (hygienist or periodontist) to remove the build-up and deposits to give you a “clean slate”.
If left and the plaque continues to build up it is likely that the gingivitis will become more established and could progress and turn into periodontitis.
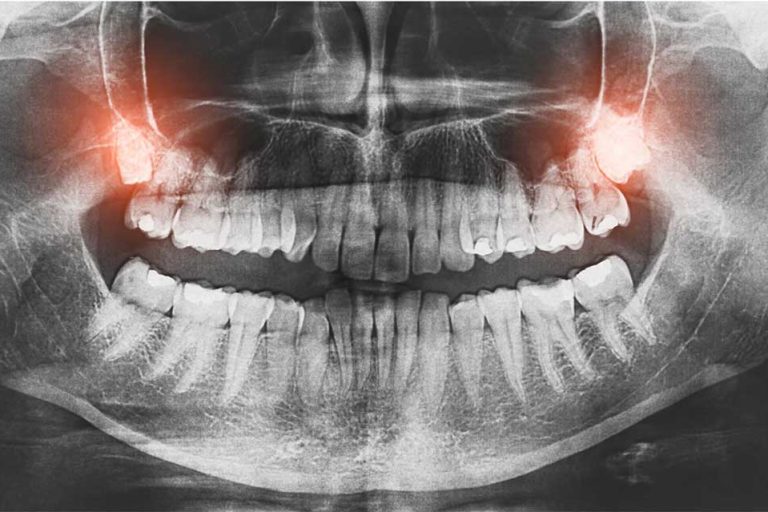
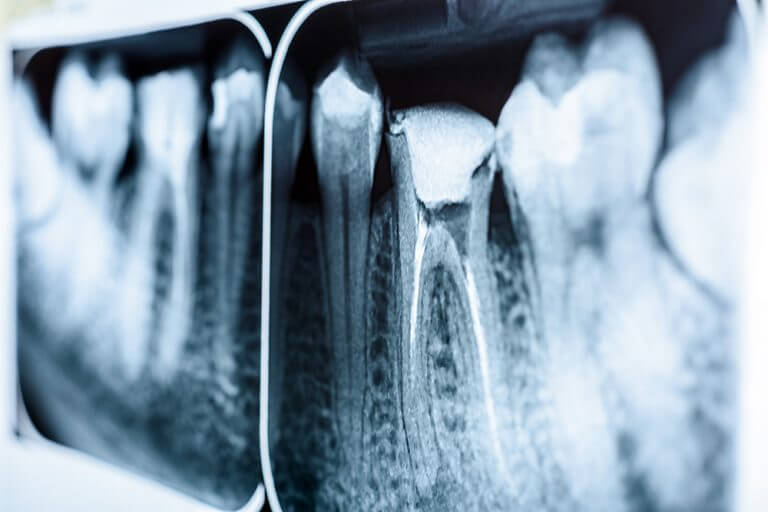
This can lead to gum loss (recession or gum pockets) and bone loss (as seen on x-rays) ultimately leading to loss of the tooth.
How do I prevent gum disease?
An excellent twice daily oral hygiene regime is required, including:
General toothbrushing twice daily, ideally cleaning with a high-quality electric toothbrush, for at least 2 minutes.
Cleaning between the teeth or interdental cleaning with floss, or interdental brushes at least once a day. The correct interdental aid mostly depends on the size and shape of the space between the teeth, and so talk to your hygienist or periodontist about what to use where properly.
Additional oral hygiene aids may be recommended such as:
- Single tufted brushes,
- Water flossers,
- Modified floss (such as SuperFlossTM or X-Floss TM),
- Tongue cleaners.
This is particularly important for cleaning plaque bacteria in specific situations such as, tilted teeth, crowded teeth, bridges, single implants, connected implants (all on four, all on six).
Your periodontist, hygienist or dentist will determine how and how frequently you will need to have your teeth professionally cleaned. Typically, intervals been appointments can be every month, to every 3 months or even up to twice a year. It is important to understand that practically it can be hard to clean all of the plaque from every site in your mouth each day, so regular hygienist visits (every 6 months) are important, even for those patients that are excellent at maintaining their own oral hygiene.
Gum disease treatment
Gingivitis may be totally reversed to health by removing the plaque bacteria that attach to your gums and teeth daily. This should be supplemented by seeing the hygienist regularly to remove hard calculus deposits on the teeth.
When you visit your dentist, he/she will advise you if you are healthy, have gingivitis or periodontitis and a programme of prevention (if your gums are already healthy) or disease management (if you have gum disease in form of gingivitis or periodontitis) will be arranged for you.
Your dentist, hygienist or periodontist can explain the most effective methods of home care for you and if the early gum disease (gingivitis) state has progressed to periodontitis (which is more advanced).
For periodontitis (gum disease with bone loss) you will need additional treatment, often by a periodontist (gum expert or specialist). The extent and severity of disease is determined by a thorough assessment to exactly determine what stage of gum disease you have, and an onward referral to a specialist periodontist is made to best manage care.
When should I seek expert help?
Bleeding is a sign of infection; healthy gums do not bleed. Other later signs of gum disease may also include teeth moving, drifting, wobbling, or tilting (especially if they were straight before), gum recession, and tooth loss. If you notice your gums bleed when you brush (or have any of the other signs), contact us for an assessment.
Call 020 3925 3846 or fill in our form to enquire about your consultation.