How To Tell If You Have Gingivitis or Periodontitis Disease
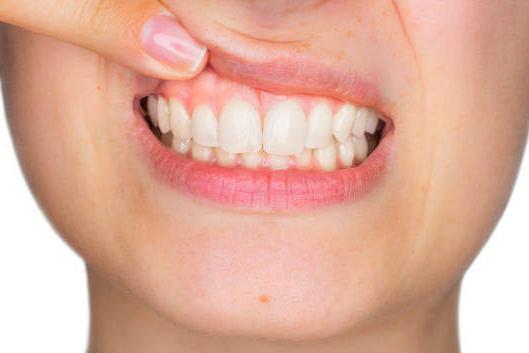
Gingivitis comes about due to the short-term consequences of plaque accumulating on your teeth, and this can cause inflammation. This inflammation usually entails red or swollen gums and bleeding when brushing teeth or biting food and is the body’s reaction to bacteria that has built up on the teeth.
If the aforementioned gingivitis is not dealt with then periodontitis can occur, this is a severe gum infection which damages the soft tissue. It can also damage the bone that supports your teeth if left untreated and subsequently lead to teeth loosening and eventually tooth loss. Let us take a closer look at the symptoms associated with both diseases so you know what to look out for
The symptoms of gingivitis and Periodontitis
There are various symptoms of gingivitis and some of these include:
- Gums bleeding when brushed or during flossing
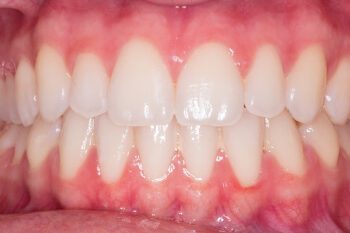
- Gums becoming a bright red or purple colour
- Gums are sore when touched
- Inflammation of the gums
- Gums appear shiny
- Halitosis
Alongside the aforementioned symptoms of gingivitis which can also apply to those with periodontitis, there are several further symptoms of periodontitis. These can vary based on the stage of periodontitis that an individual has reached, and include:
What are the risks associated with these diseases?
There are several risk factors for gingivitis, among these are:
- Certain infections and systemic diseases
- Bad oral hygiene
- Hormonal changes that occur during pregnancy
- Diabetes, especially if not controlled
- Smoking, especially if a heavy smoker
- Misalignment of teeth, fillings with rough edges, poorly fitted dental appliances, or a failure to properly maintain dental appliance
- Utilisation of certain medicines, such as phenytoin or bismuth
- Genetics
The risk factors for periodontitis are similar to gingivitis, although some additional risk factors more specific to periodontitis are:
- Obesity, especially if not controlled
- Issues related to the immune system, including HIV and leukaemia
- Genetics
- Nutritional deficiencies, such as a deficiency in vitamin C
Gingivitis and Periodontitis Disease Treatment
The best treatment for gingivitis is to make changes to your daily habits, essential to this is brushing your teeth at least twice a day, flossing daily and using mouthwash. Additionally, regular dental and hygienist visits should occur, as well as professional treatment for issues such as misaligned teeth.
Periodontitis on the other hand will require different treatment, and this is also based on the severity of your condition. In some scenarios your dentist can recommend non-invasive procedures such as a scaling to remove build-up on your teeth and below your gum line. This can also include root planing which discourages plaque build-up by smoothing out the surface of the roots of your teeth. If the gum infections remain and they aren’t responding to professional hygiene, then antibiotics may need to be prescribed.
Surgery can be required if the inflammation still persists in sites which are inaccessible to brushing and flossing. This can be in the form of flap surgery, in which the deposits under your gums are cleaned. Additionally, if you have had bone loss then bone grafting may be carried out with the flap surgery, in order to restore the lost bone.
If you would like further advice on either condition, our practice is committed to educating patients manage gum disease as it is the UK’s leading cause of tooth loss. Please do get in contact with us if you want to know more about either of the conditions mentioned in this article.
Call 020 3925 3846 or fill in our form to enquire about your consultation.